The Vagus Nerve and Your Gut: The Missing Link to Midlife GI Wellness (Especially on GLP-1s)
- Posted by Raven Meyers
- Categories GLP-1 Support, Gut Health, Wellness and Mid-Life Health
- Date November 11, 2025
For women navigating midlife
Especially those on GLP-1 medications like semaglutide or tirzepatide, the digestive system can feel unpredictable. Bloating, constipation, nausea, or slowed motility are common. Few realize that one “wandering” nerve deeply influences these experiences: the vagus nerve. Understanding and supporting this nerve can profoundly improve gut function, stress response, and how your body adapts to GLP-1 therapy.
What Is the Vagus Nerve?
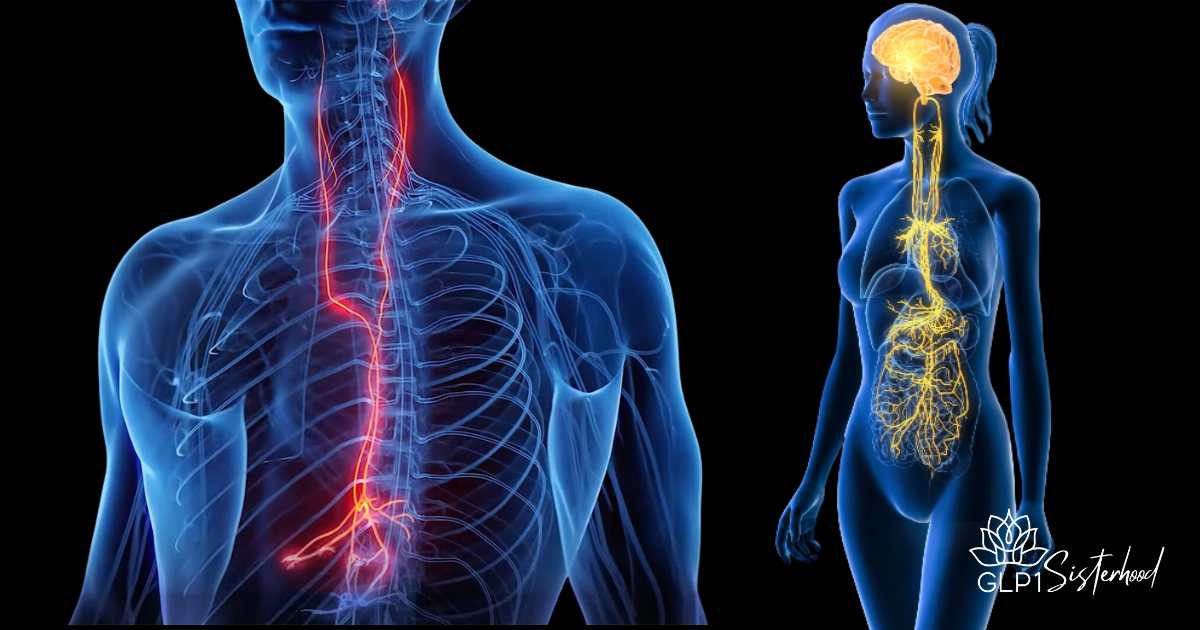
The vagus nerve (cranial nerve X) is the longest cranial nerve in the body. It travels from the brainstem through the neck and thorax to the abdomen, connecting the brain to organs including the heart, lungs, and gastrointestinal (GI) tract.
It’s a central component of the parasympathetic nervous system, often called the “rest and digest” system, counterbalancing the stress-driven “fight or flight” response.
When the vagus nerve functions well, digestion, heart rate, inflammation, and emotional regulation are in harmony. When it’s underactive, symptoms like poor digestion, bloating, constipation, or anxiety may emerge.
Key evidence:
- The vagus nerve regulates intestinal motility, enzyme secretion, and gut permeability (Breit, Kupferberg et al., Frontiers in Psychiatry, 2018).
- Low vagal tone is associated with irritable bowel symptoms and chronic inflammation (Bonaz & Pellissier, Neurogastroenterology & Motility, 2016).
The Gut-Brain Connection: How the Vagus Nerve Communicates
The vagus nerve serves as a bi-directional communication pathway between the gut and brain known as the gut-brain axis.
Up to 80% of vagal fibers carry sensory information from the gut to the brain (Bonaz et al., 2018). This means your emotional and physical state directly affect digestion, and digestive imbalance can impact mood, energy, and cognition.
When vagal tone is high: digestion flows, nutrients are absorbed efficiently, and inflammation is controlled.
When vagal tone is low: gut motility slows, causing nausea, reflux, constipation, or bloating.
Why the Vagus Nerve Matters on GLP-1s
GLP-1 receptor agonists (like semaglutide, liraglutide, or tirzepatide) work by slowing gastric emptying and improving insulin sensitivity. Which is helpful for blood sugar and appetite regulation, but sometimes uncomfortable for digestion.
The vagus nerve interacts directly with GLP-1 pathways:
- GLP-1 activates vagal afferent neurons in the gut to signal satiety to the brain (Holst, Nature Reviews Endocrinology, 2019).
- Chronic stress or low vagal tone can impair this communication, worsening nausea or fullness sensations.
- A healthy vagus nerve supports gastric motility and helps mitigate GLP-1–related constipation and discomfort (Yamamoto et al., American Journal of Physiology, 2010).
In short:
Supporting your vagal tone can ease GLP-1 side effects and enhance how effectively the medication works with your body—not against it.
How the Vagus Nerve Supports the GI System
- Gastric Motility
Stimulates smooth muscle contractions that move food through the digestive tract (Bonaz, 2018). - Digestive Secretions
Enhances enzyme and bile secretion to aid nutrient breakdown. - Anti-inflammatory Effects
Activates the “cholinergic anti-inflammatory pathway,” reducing systemic inflammation linked to gut discomfort and autoimmune risk (Tracey, Nature Reviews Immunology, 2002). - Gut Barrier Protection
Helps maintain tight junction integrity, preventing “leaky gut” and related inflammation (Breit et al., 2018).
Ways to Strengthen and Support the Vagus Nerve
- Deep, Slow Breathing
Research shows slow exhalation breathing improves vagal tone and heart rate variability (Jerath et al., Frontiers in Human Neuroscience, 2019). Try 4-count inhale, 6-count exhale breathing for 5 minutes daily. - Cold Exposure
Brief facial cold exposure activates vagal parasympathetic responses (McCraty & Shaffer, Frontiers in Psychology, 2015). - Singing, Humming, Chanting
Vocalization stimulates vagal activity through the laryngeal branch of the nerve. Studies link chanting and humming to reduced heart rate and improved mood (Kalyani et al., International Journal of Yoga, 2011). - Mindful Eating and Chewing Slowly
Vagal signals begin with sensory cues of food—smell, taste, and chewing—stimulating salivary and digestive enzyme release (Bonaz & Pellissier, 2016). - Gentle Movement and Yoga
Yoga and tai chi are shown to enhance parasympathetic tone and lower cortisol (Streeter et al., Medical Hypotheses, 2012). - Stress Reduction and Emotional Safety
Chronic stress suppresses vagal tone. Journaling, therapy, community support, and relaxation rituals rebuild nervous system resilience (Porges, The Polyvagal Theory, 2011).

Affirmation
“I trust my body’s wisdom. Each breath restores balance, each meal becomes medicine, and I am safe in my healing rhythm.”
Final Thought
The vagus nerve is your internal peacekeeper, bridging the emotional, hormonal, and digestive worlds. For women on GLP-1s, nurturing this nerve is a gentle yet powerful way to restore harmony to your gut and nervous system. Healing isn’t just about medication; it’s about restoring communication between body and brain.
Invitation To Our Membership
Soul to Soul Sisterhood™ is a sanctuary for midlife women and all who identify as women who are seeking steadiness, healing, and meaning in a modern world.
This is our foundational membership for women integrating weight loss, metabolic healing, emotional well-being, and spiritual grounding into everyday life. For those using GLP-1 medications, optional focused support is available through a dedicated pathway within the sisterhood.
This is not a space for urgency or perfection.
It is a place to arrive, to integrate, and to remain supported as life unfolds.

Sources
- Bonaz, B., & Pellissier, S. (2016). The Vagus Nerve at the Interface of the Microbiota–Gut–Brain Axis. Neurogastroenterology & Motility.
- Breit, S., Kupferberg, A., Rogler, G., & Hasler, G. (2018). Vagus Nerve as Modulator of the Brain–Gut Axis in Psychiatric and Inflammatory Disorders. Frontiers in Psychiatry, 9:44.
- Holst, J.J. (2019). The Physiology of GLP-1 and GLP-1-based Therapies. Nature Reviews Endocrinology, 15, 717–738.
- Tracey, K.J. (2002). The Inflammatory Reflex. Nature Reviews Immunology, 2(6), 415–426.
- Yamamoto, H., Lee, C.E., Marcus, J.N., Williams, T.D., Overton, J.M., Lopez, M.E. et al. (2010). GLP-1 Receptor Stimulation and Vagal Afferents Regulate Gastric Motility and Emptying. American Journal of Physiology-Gastrointestinal and Liver Physiology, 298(6): G981–G987.
- Jerath, R., Edry, J.W., Barnes, V.A., & Jerath, V. (2019). Physiology of Long Pranayamic Breathing: Neural Cardiorespiratory Synchronization. Frontiers in Human Neuroscience, 13:425.
- McCraty, R., & Shaffer, F. (2015). Heart Rate Variability: New Perspectives on Assessment and Training. Frontiers in Psychology, 6:43.
- Kalyani, B.G., Venkatasubramanian, G., Arasappa, R. et al. (2011). Neurohemodynamic Correlates of ‘OM’ Chanting: A Pilot Functional MRI Study. International Journal of Yoga, 4(1):3–6.
- Streeter, C.C., Gerbarg, P.L., Saper, R.B., Ciraulo, D.A., & Brown, R.P. (2012). Effects of Yoga on the Autonomic Nervous System, Gamma-Aminobutyric-Acid, and Allostasis in Epilepsy, Depression, and PTSD. Medical Hypotheses, 78(5):571–579.
- Porges, S.W. (2011). The Polyvagal Theory: Neurophysiological Foundations of Emotions, Attachment, Communication, and Self-Regulation. W.W. Norton & Co.
Raven Meyers is a wife and mother, a learning architect, Industrial design engineer and educator. The founder of Soul to Soul Sisterhood™, The Scrub Ninjas™, and EDTECH EDU™. For the last thirty years, she has been building spaces of learning, healing, and connection, guided by both lived experience and deep listening.
Her work is shaped by a rare convergence of disciplines, including holistic midwifery, Eastern medicine, instructional design, and global entrepreneurship. Through this integration, Raven creates environments that honor the body, calm the nervous system, and restore trust in the self, particularly for women navigating midlife transitions.
At the heart of her work is a devotion to women over forty who are ready to move beyond shame, urgency, and isolation. Through sisterhood, soulful practices, and evidence-based education, Raven supports women in reclaiming their relationship with their bodies, their health, and their inner wisdom.
Whether she is designing learning ecosystems, tending family life, or holding sacred circles, Raven brings steadiness, compassion, and integrity to all she creates.